
Can we really prevent injury? Many people get all bent out of shape when they hear the words: injury prevention. I have had people get pretty upset with me because I have a publicity that runs for the Movement Optimization for Prehab & Performance Course that uses those exact words. I actually had someone write to me on Instagram to tell me he was unfollowing me because I used the term. Oh well.
Enjoyed this video? Subscribe to our YouTube channel!
The truth is that if you train or take part in any sport, you subject yourself to potential injury. Everyone who partakes in physical activity needs to be willing to take that risk. In sports and training, injury comes with the territory.
When I talk about injury prevention, I’m not claiming that all injuries can be prevented. Certainly, if you catch a 300-lb clean wrong and injure your knee, it’s not because your glute med was shut down and I won’t tell you that you could have prevented that by including clamshells in your training regimen. Accidents and acute injuries happen, that is reality. With sport specialization, even overuse injuries are hard to prevent.
Injury prevention is a term that refers to implementing structure and strategies that reduce injury risk, occurrence and severity
by improving robustness and resilience. This involves appropriate programming and periodization to ensure that sufficient recovery is allowed. Additional strategies include optimizing fundamental movement to ensure proper load distribution and avoid excessive or repetitive stress, which can lead to injury.
ROBUSTNESS AND RESILIENCE
Sports injury prevention programs rely on neuromuscular training as a means to reduce the risk of injury, and there is evidence that this is effective in reducing the incidence of certain injuries.
Training programs should focus on motor control and strength to improve robustness and resilience. We often hear these terms used interchangeably and both are important from a rehabilitation perspective.
A robust tissue can tolerate more load without deformation. It can tolerate higher loads without giving. Think of a bullet bouncing off a bulletproof window. From a training perspective, think of the body’s ability to handle high loads. Strength is important in ensuring robustness.
A resilient tissue can bend without breaking. It can tolerate deformation and return to its function unscathed. Think of a palm tree bending with the wind and standing straight on a windless day. From a training perspective, think of the body’s ability to handle loads applied differently. I often explain this as the ability to display strength in less than perfect positions.
HOW INJURIES OCCUR
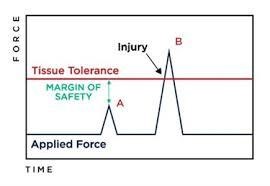
Musculoskeletal injury occurs through exposure to physical stress and is dependent on the magnitude and time of application of that stress. Excessive physical stress causes injury through any of the following 3 mechanisms:
- A high-magnitude stress applied for a brief period (acute injury such as a sprain, strain or fracture) that surpasses the physiological limit of the tissue
- A lower magnitude stress applied for a long duration that lowers the tissue’s tolerance
- A lower magnitude stress applied to the tissue repetitively that lowers the tissue’s tolerance
On the other hand, we know that stress on tissue within physiological limits and with sufficient recovery normally leads to tissue adaptation.
This means that factors that increase the magnitude of stress on the tissue or have an impact on the time required for the tissue to recover sufficiently, may result in an associated risk or occurrence of injury. As such, these are factors worth exploring in an injury prevention program.
TARGETING RISK FACTORS
In identifying injury risk factors, there will be both extrinsic and intrinsic athlete risk factors. Extrinsic factors are specific to the sport or training you are dealing with. For example, contact sports have different extrinsic factors than non-contact sports, high-demand overhead sports have a shoulder injury risk, etc.
Let’s take the shoulder as an example. We know that impingement is a natural physiological process that occurs when we move the upper extremity overhead. However, with high-demand overhead sport, this occurs more frequently and often under load. These are extrinsic factors that we need to take into consideration, and this is generally done with appropriate programming and periodization to ensure that sufficient recovery is allowed.
Intrinsic factors are athlete specific. Things like previous injury, strength, motor control, mobility. Many of these intrinsic factors can contribute to excessive overload of the shoulder even with appropriate programming. For example, limited scapulothoracic movement could create additional impingement and impact recovery and tissue tolerance. Hypermobility can result in occult instability, subluxations that the athlete is not even aware of, that lead to excessive accessory movement and potential injury. A previous injury may result in decreased movement variability, decreased mobility, accessory movement deficits, many of which will go unnoticed until sometimes the opposite shoulder starts to bear the excessive load.
MOVEMENT OPTIMIZATION
Factors like proprioception, neuromuscular control, mobility and strength have been hypothesized to be associated with injury risk. The Movement Optimization for Prehab and Performance strategy is primarily focused on optimizing fundamental movement to address and modify these risk factors.
For example, at a very basic level, a stable loaded overhead position requires upward rotation and posterior tilt of the scapula, thoracic spine extension and reactive anterior core stabilization. You can screen for this using the bilateral shoulder flexion test. I have written an article on this, as well as a two-part article on Prerequisites for Overhead Lifting: Part 1 and Part 2.
Deficits in fundamental movement can stem from the many different factors that have been hypothesized to be associated with increased injury risk: myofascial restrictions of the scapular or glenohumeral muscles, articular restrictions, motor control, muscle strength, or a mix of several of these factors.
Although there is no consensus about the cause–consequence relationship of movement mechanics and pain, if you combine deficits in range of motion with a high-demand overhead activity, you get greater opportunity for greater impingement stress and thus, a higher risk of exceeding tissue tolerance. I have seen it in practice over and over again.
This is why in my practice, restoring fundamental movement comes first, whether or not there has been pain or injury, or not.
A STRATEGY FOR PREVENTION
So, can we really prevent injury?
Just like movement optimization, prevention is a strategy. Within this strategy we need to identify what the etiologies and mechanisms of injuries are and what strategies may help prevent the incidence and severity of these injuries. As with any strategy, compliance and sustainability are important. Here is a great article from The Prehab Guys that talks about selecting prehab exercises based on the specific demands and common injuries in soccer.
Sports and physical activity subject our clients to the risk of injury. But just like there are variables of injury that we cannot control, there are those that we can control. Movement optimization is about implementing structure and strategies that reduce injury risk, occurrence and severity by addressing deficits in proprioception, neuromuscular control, mobility and strength, which have been hypothesized to be associated with injury risk.
So, yes, we can really prevent injury. Or, if you want to argue semantics, we can reduce or mitigate the risk of injury with appropriate and sustainable programming. This is already a better service to your clients than doing nothing at all under the claim that there is no proven cause–consequence relationship between optimal movement and injury risk.
REFERENCES:
Cools, A., Struyf, F., De Mey, K., Maenhout, A., Castelein, B., & Cagnie, B. (2013). Rehabilitation of scapular dyskinesis: from the office worker to the elite overhead athlete. British Journal Of Sports Medicine, 48(8), 692-697. doi: 10.1136/bjsports-2013-092148
Emery, C., Roy, T., Whittaker, J., Nettel-Aguirre, A., & van Mechelen, W. (2015). Neuromuscular training injury prevention strategies in youth sport: a systematic review and meta-analysis. British Journal Of Sports Medicine, 49(13), 865-870. doi: 10.1136/bjsports-2015-094639
van Mechelen, W., Hlobil, H., & Kemper, H. (1992). Incidence, Severity, Aetiology and Prevention of Sports Injuries. Sports Medicine, 14(2), 82-99. doi: 10.2165/00007256-199214020-00002

Mai-Linh Dovan M.SC., CAT(C)
Certified Athletic Therapist
Founder of Rehab-U







… [Trackback]
[…] Find More on on that Topic: rehab-u.com/injury-prevention-is-it-a-myth/ […]
… [Trackback]
[…] Find More here on that Topic: rehab-u.com/injury-prevention-is-it-a-myth/ […]
… [Trackback]
[…] Read More on that Topic: rehab-u.com/injury-prevention-is-it-a-myth/ […]
… [Trackback]
[…] Info to that Topic: rehab-u.com/injury-prevention-is-it-a-myth/ […]
… [Trackback]
[…] Info to that Topic: rehab-u.com/injury-prevention-is-it-a-myth/ […]
… [Trackback]
[…] Information to that Topic: rehab-u.com/injury-prevention-is-it-a-myth/ […]
… [Trackback]
[…] Read More on that Topic: rehab-u.com/injury-prevention-is-it-a-myth/ […]
… [Trackback]
[…] There you will find 47092 more Info on that Topic: rehab-u.com/injury-prevention-is-it-a-myth/ […]
… [Trackback]
[…] Find More Info here to that Topic: rehab-u.com/injury-prevention-is-it-a-myth/ […]
… [Trackback]
[…] Find More Information here on that Topic: rehab-u.com/injury-prevention-is-it-a-myth/ […]
… [Trackback]
[…] Read More on to that Topic: rehab-u.com/injury-prevention-is-it-a-myth/ […]
… [Trackback]
[…] Information on that Topic: rehab-u.com/injury-prevention-is-it-a-myth/ […]
… [Trackback]
[…] There you can find 52439 additional Info to that Topic: rehab-u.com/injury-prevention-is-it-a-myth/ […]
… [Trackback]
[…] Find More Info here on that Topic: rehab-u.com/injury-prevention-is-it-a-myth/ […]
… [Trackback]
[…] Find More on that Topic: rehab-u.com/injury-prevention-is-it-a-myth/ […]
… [Trackback]
[…] Find More Info here to that Topic: rehab-u.com/injury-prevention-is-it-a-myth/ […]
… [Trackback]
[…] Find More on to that Topic: rehab-u.com/injury-prevention-is-it-a-myth/ […]
… [Trackback]
[…] Read More to that Topic: rehab-u.com/injury-prevention-is-it-a-myth/ […]
… [Trackback]
[…] Find More Information here to that Topic: rehab-u.com/injury-prevention-is-it-a-myth/ […]
… [Trackback]
[…] Read More Info here to that Topic: rehab-u.com/injury-prevention-is-it-a-myth/ […]
… [Trackback]
[…] Information to that Topic: rehab-u.com/injury-prevention-is-it-a-myth/ […]
… [Trackback]
[…] Find More to that Topic: rehab-u.com/injury-prevention-is-it-a-myth/ […]
… [Trackback]
[…] Find More Info here to that Topic: rehab-u.com/injury-prevention-is-it-a-myth/ […]
… [Trackback]
[…] Find More on that Topic: rehab-u.com/injury-prevention-is-it-a-myth/ […]
… [Trackback]
[…] Find More Information here on that Topic: rehab-u.com/injury-prevention-is-it-a-myth/ […]
… [Trackback]
[…] Find More Information here to that Topic: rehab-u.com/injury-prevention-is-it-a-myth/ […]
… [Trackback]
[…] Find More to that Topic: rehab-u.com/injury-prevention-is-it-a-myth/ […]
… [Trackback]
[…] Find More on to that Topic: rehab-u.com/injury-prevention-is-it-a-myth/ […]
… [Trackback]
[…] Find More on to that Topic: rehab-u.com/injury-prevention-is-it-a-myth/ […]
… [Trackback]
[…] Info to that Topic: rehab-u.com/injury-prevention-is-it-a-myth/ […]