
Stop stretching for tendinopathy! It may actually make your pain worse. Many people who come see me with tendinopathy have been given stretches to alleviate muscle tension, which is assumed to be contributing to their pain. However, there are a couple of problems with this. For one, tendons don’t need stretch, they need stiffness.
Second, and perhaps a more important problem, is that stretches result in compression of the tendon and tendinopathic tendons don’t like compression. For example, stretching the quad requires knee flexion which results in compression of the quad tendon over the femoral condyle; stretching the glutes requires adduction which results in compression of the glute med tendon over the greater trochanter; stretching the hamstrings requires hip flexion which compresses the tendon over the ischial tuberosity.
If you have been in the habit of prescribing stretches for tendon pain, this may be perpetuating the injury. It is time to upgrade to a more efficient strategy.
Understanding compressive load in tendinopathy and how to manage it is crucial to designing the most optimal intervention and to avoid exacerbating pain and pathology.
Enjoyed this video? Make sure to subscribe to our YouTube channel!
TENDINOPATHY
Tendinopathy is an umbrella term that indicates a non-rupture injury of the tendon that is exacerbated by mechanical loading. It is often described as a failed healing response. When you overload a healthy tendon, you move it from a healthy state to an injured stated, much like when you train a muscle. This process is normal and essential. However, without appropriate recovery, the tendon cell stays metabolically primed and reacts to minimal activity, starting the cycle of failed healing.
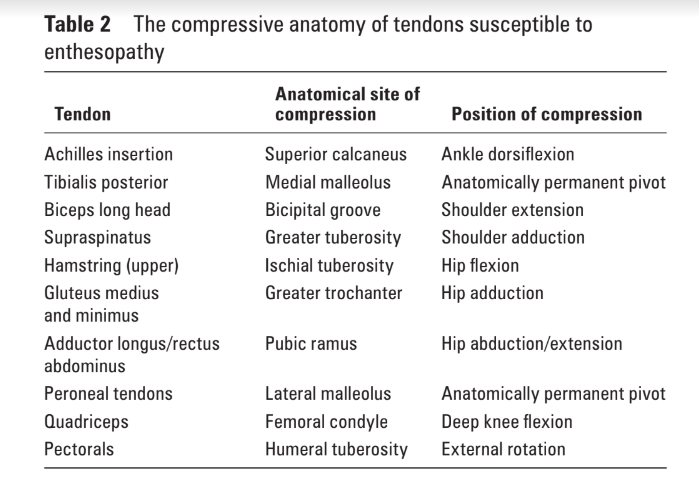
Recent studies strongly suggest that compression where bone and tendon approximate is an important consideration in the onset of tendinopathy. Compression of a tendon occurs when it is squeezed along the bony protuberance near or at the joint. Compression in itself may have minimal effects on tendons, but the combination of compressive and tensile loads is proposed to be particularly damaging to tendons. For example, an exercise like a lunge produces a quadriceps contraction and tensile load on the patellofemoral tendon. The more the knee moves forward over the toes, the more the compressive load is also increased.
As suggested by Cook and Purdham (2012), tendons that have a bony prominence proximal to the insertion, are nearly always exposed to both tensile and compressive loads, especially in certain joint positions.
Understanding this is important, because managing load for tendon pain needs to include both tensile and compressive loads. Manipulating joint positions with specific exercise variations can help decrease compressive load. Here are some examples of how you might achieve this:
IF NOT STRETCHING, THEN WHAT?
Most of the stretches that are prescribed to address tendon pain result in compression of the tendon over the distal bony protuberance. For example, a quad stretch will result in compression of the quad tendon over the femoral condyle. The problem is that a tendinopathic tendon becomes mechanically sensitive, and as such,
Even the compression from a static stretch can be painful and detrimental to the healing process
That said, there certainly may be soft tissue limitations contributing to tendon overload. Managing tendinopathy is as much about the tendon as it is about muscle-tendon unit function. Tendons reduce muscular work by storing and releasing elastic energy. On the flip side, the tendon depends on the muscle to protect it via efficient deceleration capacity, or better said, eccentric strength. This is one of the reasons why eccentrics are so often employed for the management of tendinopathy.
This muscle-tendon coordination is an important factor to consider, which means that if there is muscle tension, it will need to be managed. Because we want to avoid the compression of static stretching, myofascial release techniques are the best option here, treating the belly of the muscle and avoiding the area of the tendon. Cupping techniques, if you have access to them, are interesting because they release the tissue by lifting it rather than compressing it. If you are working with a client who has been accustomed to rolling and smashing, changing it up with the use of cupping may be especially effective because it creates a different stimulus.
DECELERATION AND CONTROL
Decreased control of foot pronation and eversion of the subtalar joint may contribute to suboptimal deceleration mechanics, and I often see this in cases of Achilles and patellofemoral tendinopathy. In these cases, working on deceleration and control needs to start with restoring foot stability. For some strategies to work on this component, head to this article on my blog: Foot Stability is the Foundation for all Your Lifts. Perhaps the most important choice you will need to make in your intervention is selecting exercises that can address the eccentric component of deceleration while still managing compressive load
As we have discussed earlier, the resultant compressive force on the patellofemoral tendon increases as knee flexion angle increases, even with passive knee flexion. Again, this is why even passive stretching can be irritable and should be avoided. We also outline that with quadriceps contraction, such as in a lunge, the compressive force increases additionally. This means that you will need to select exercises in specific joint positions so that you can simultaneously eccentrically load the tendon and control compressive load.
The step-down, a classic rehab exercise used for both Achilles as well as patellofemoral tendinopathy, is a great example of an exercise that you can modify quite easily. By manipulating where the non-support foot steps down, you can decrease and progressively increase the moment arm at the knee to manage the amount of quad contraction and its effect on compressive load. Specifically, there will be less compressive load if the client steps down with the non-support behind and then increasingly more compressive load if they step down beside, then in front of the support foot.
You can also manipulate classic training exercises to suit the needs of the rehabilitation process. For example, using a forward lunge where the knee is not allowed to go past the toes and progressively letting the knee come forward. The objective here is not only to progressively subject the tendon to more compressive load, but also to progressively increase the deceleration demand of the exercise.
Watch the main video of the article to see how these exercises are done.
Another progression I like to use initially is to let the knee come forward but with a variation that is a little less quad dominant, like a reverse lunge. Here is an example of a landmine reverse lunge performed using an external pace. Make sure you read about externally paced exercise for the management of tendinopathy in my previous article: Knee Pain Management for Effective Results.
STOP STRETCHING
For years people have been trying to manage tendinopathy through stretching and this needs to change. In fact, the more severe the tendinopathy, the less likely it is that stretching will be beneficial.
A better understanding of compressive load is an important factor in the management of tendinopathy. Tendons that have a bony protuberance proximal to their insertion, like for example the Achilles, patellofemoral and hamstring tendons, are nearly always exposed to tensile and compressive loads. Care needs to be taken to manage these loads by adjusting and controlling joint positions via exercise modifications.
If you want to make real progress with tendinopathy, all of these elements of training need to be part of your rehab plan!
Enjoyed this article? Subscribe to our YouTube channel!
REFERENCES:
Witvrouw, E., Mahieu, N., Roosen, P., & McNair, P. (2007). The role of stretching in tendon injuries. British Journal Of Sports Medicine, 41(4), 224-226. doi: 10.1136/bjsm.2006.034165
Cook, J., & Purdam, C. (2011). Is compressive load a factor in the development of tendinopathy? British Journal Of Sports Medicine, 46(3), 163-168. doi: 10.1136/bjsports-2011-090414

Mai-Linh Dovan M.SC., CAT(C)
Certified Athletic Therapist
Founder of Rehab-U





… [Trackback]
[…] Read More to that Topic: rehab-u.com/stop-stretching-for-tendinopathy/ […]
… [Trackback]
[…] Read More on that Topic: rehab-u.com/stop-stretching-for-tendinopathy/ […]
… [Trackback]
[…] Find More on that Topic: rehab-u.com/stop-stretching-for-tendinopathy/ […]
… [Trackback]
[…] Find More Information here on that Topic: rehab-u.com/stop-stretching-for-tendinopathy/ […]
… [Trackback]
[…] Read More on to that Topic: rehab-u.com/stop-stretching-for-tendinopathy/ […]
… [Trackback]
[…] Find More here on that Topic: rehab-u.com/stop-stretching-for-tendinopathy/ […]
… [Trackback]
[…] Find More here on that Topic: rehab-u.com/stop-stretching-for-tendinopathy/ […]
… [Trackback]
[…] Read More Info here on that Topic: rehab-u.com/stop-stretching-for-tendinopathy/ […]
… [Trackback]
[…] Find More to that Topic: rehab-u.com/stop-stretching-for-tendinopathy/ […]
… [Trackback]
[…] Find More Info here on that Topic: rehab-u.com/stop-stretching-for-tendinopathy/ […]
… [Trackback]
[…] Read More Information here on that Topic: rehab-u.com/stop-stretching-for-tendinopathy/ […]
… [Trackback]
[…] Read More to that Topic: rehab-u.com/stop-stretching-for-tendinopathy/ […]
… [Trackback]
[…] Find More Information here to that Topic: rehab-u.com/stop-stretching-for-tendinopathy/ […]
… [Trackback]
[…] Here you will find 52102 additional Info to that Topic: rehab-u.com/stop-stretching-for-tendinopathy/ […]
… [Trackback]
[…] Read More here on that Topic: rehab-u.com/stop-stretching-for-tendinopathy/ […]
… [Trackback]
[…] Information on that Topic: rehab-u.com/stop-stretching-for-tendinopathy/ […]
… [Trackback]
[…] Here you can find 85261 more Information on that Topic: rehab-u.com/stop-stretching-for-tendinopathy/ […]
… [Trackback]
[…] Read More to that Topic: rehab-u.com/stop-stretching-for-tendinopathy/ […]
… [Trackback]
[…] Here you can find 78531 more Info to that Topic: rehab-u.com/stop-stretching-for-tendinopathy/ […]
… [Trackback]
[…] There you will find 93892 additional Information to that Topic: rehab-u.com/stop-stretching-for-tendinopathy/ […]
… [Trackback]
[…] Read More on that Topic: rehab-u.com/stop-stretching-for-tendinopathy/ […]
… [Trackback]
[…] Read More Information here to that Topic: rehab-u.com/stop-stretching-for-tendinopathy/ […]
… [Trackback]
[…] Find More here to that Topic: rehab-u.com/stop-stretching-for-tendinopathy/ […]
… [Trackback]
[…] Here you will find 35257 more Information to that Topic: rehab-u.com/stop-stretching-for-tendinopathy/ […]
… [Trackback]
[…] Read More Information here to that Topic: rehab-u.com/stop-stretching-for-tendinopathy/ […]
… [Trackback]
[…] Read More here on that Topic: rehab-u.com/stop-stretching-for-tendinopathy/ […]
… [Trackback]
[…] There you will find 9044 more Information to that Topic: rehab-u.com/stop-stretching-for-tendinopathy/ […]
… [Trackback]
[…] There you will find 7951 more Info to that Topic: rehab-u.com/stop-stretching-for-tendinopathy/ […]
… [Trackback]
[…] There you will find 31518 additional Info to that Topic: rehab-u.com/stop-stretching-for-tendinopathy/ […]
… [Trackback]
[…] Find More to that Topic: rehab-u.com/stop-stretching-for-tendinopathy/ […]